The following highlights how an extremely common scenario unfolds in a stand-alone centre versus a co-located site. The hypothetical patients could be any of us or our loved ones. The details used are fictitious but standard and will be only too familiar to every medical professional who reads this
Patient S
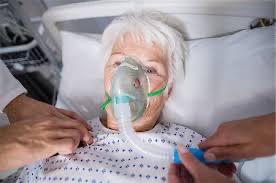
Patient S is currently attending an oncology clinic in a stand-alone cancer centre. She is 52, a librarian and lifelong smoker who enjoys walking her dog. She is going to be admitted for the management of pain and feeding problems following her radiotherapy for laryngeal cancer.
S’s husband has been trying to feed her soup and mashed potato to keep her energy up but notices that she has been coughing when she eats. The team explain that she may have been inhaling some of the food because of her abnormal swallow.
S’s prognosis is excellent and her treatment should be curative. She currently can’t cope at home because she struggles to swallow her pain killers. She is becoming dehydrated and is in severe pain. Her team have decided that she should have a tube placed for nasogastric feeding and pain relief with supportive nursing for a few days whilst they regain control of her symptoms. S is admitted to a stand-alone cancer centre, about three miles from the nearest acute hospital.
Several hours later
S is much more comfortable. She has a nasogastric tube in place so she can be fed and receive pain killers. Unfortunately, later that night, S starts to develop temperatures and a cough. The nurses notice she is becoming confused and sounds breathless. A chest x-ray shows pneumonia with the nasogastric tube in the correct location.
Continue reading